The Mind–Body Connection and the Menstrual Cycle
By Kimberley van Schagen
How stress, the nervous system and hormones shape your cycle
The menstrual cycle is a full mind–body experience. The brain and the reproductive system are in constant conversation. Your nervous system, stress responses, thoughts and emotions actively shape your hormonal landscape and vice versa.
The science behind the mind–body connection
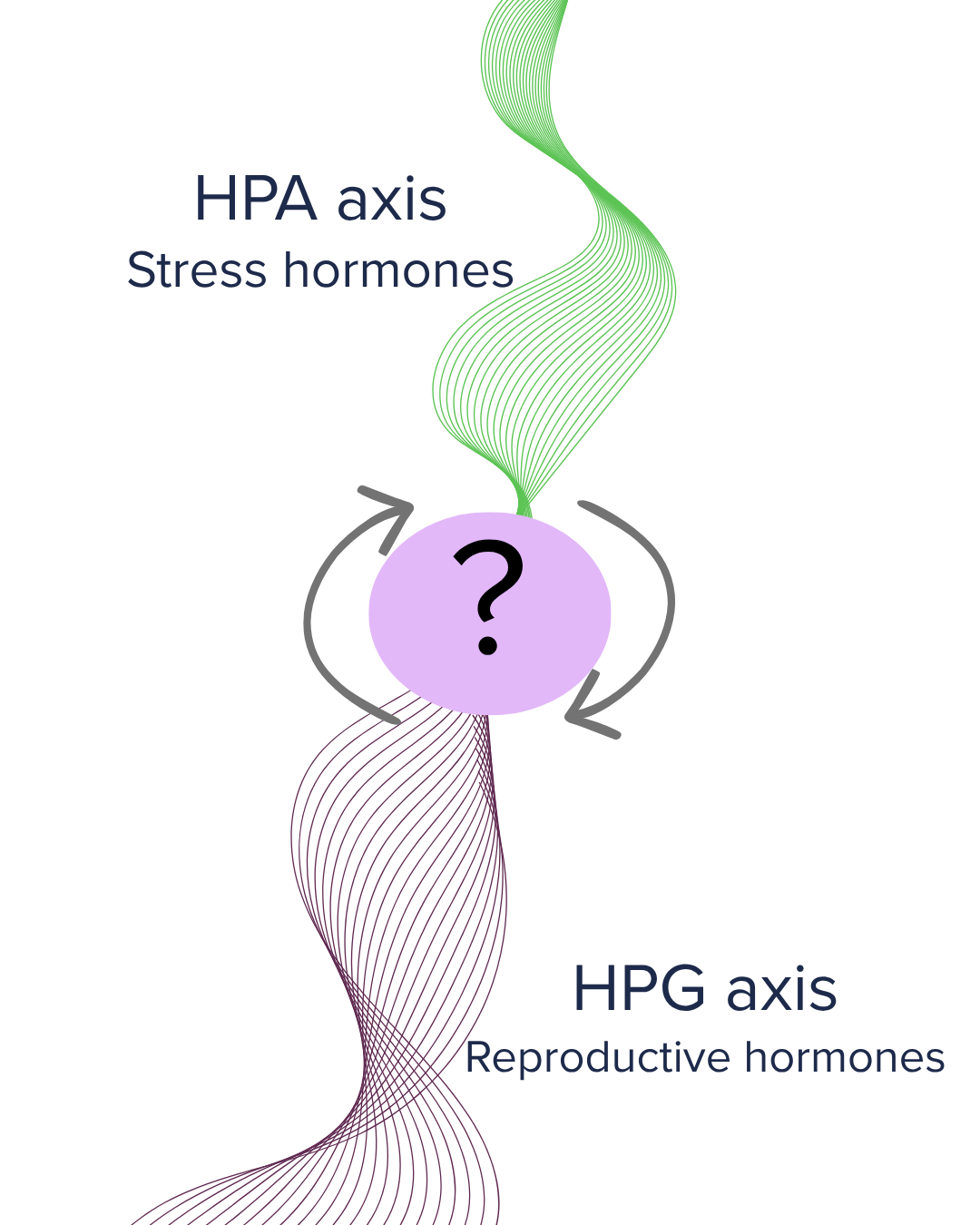
At the centre of this communication are two major systems that constantly influence each other:
The HPA axis (Hypothalamic–Pituitary–Adrenal axis), which regulates your stress response
The HPG axis (Hypothalamic–Pituitary–Gonadal axis), which regulates reproductive hormones. [1]
When your brain perceives stress (physical, emotional or psychological), the HPA axis triggers the release of cortisol, your primary stress hormone. At the same time, the hypothalamus is responsible for releasing GnRH (Gonadotropin-Releasing Hormone), which initiates the hormonal cascade required for ovulation. But chronic stress disrupts this process. Elevated cortisol levels can suppress GnRH, which in turn affects LH (Luteinizing Hormone) and FSH (Follicle-Stimulating Hormone), both essential for ovulation.[2]
How stress affects the menstrual cycle
When stress becomes chronic, the body prioritises survival over reproduction. In simple terms, it reads the environment as “not safe.”
This can lead to:
Delayed or absent ovulation
A shortened luteal phase
Irregular or missing periods (hypothalamic amenorrhea)
Increased PMS symptoms
More intense menstrual cramps (dysmenorrhea) [3][4]
You can actively support your hormonal health by working with your nervous system.
Yoga and the menstrual cycle
Yoga is a tool for regulating stress and improving body awareness.
Physiologically, yoga reduces cortisol levels and activates the parasympathetic nervous system [5] (your “rest and digest” state).
But just as importantly, it strengthens interoception (your ability to sense internal bodily signals).
People who practice yoga regularly often report better awareness of different menstrual cycle phases, reduced menstrual pain and less severe PMS symptoms.[6]
Breathwork for hormonal regulation
Breathwork is one of the fastest ways to influence your nervous system.
Techniques like slow diaphragmatic breathing or coherence breathing (around 6 breaths per minute) stimulate the vagus nerve, which helps shift the body out of stress mode. This directly downregulates the HPA axis, making breathwork a powerful tool for: reducing stress quickly, supporting hormonal balance and calming the body during high-stress or high-symptom phases.[7]
A simple place to start is belly breathing. How to do it: take slow, deep breaths that expand the abdomen rather than the chest. When you breathe into your abdomen instead of your chest, you engage the diaphragm, a large muscle connected to the vagus nerve – one of the main regulators of your stress response.
Mindfulness and cycle awareness
Mindfulness practices, including meditation, change how the brain processes stress.
They reduce activity in the amygdala (the brain’s threat detection centre), making it less reactive.[8] This matters because an overactive amygdala keeps your stress response constantly switched on.
Beyond stress reduction, mindfulness helps you notice subtle shifts across your cycle, understand your body’s patterns and respond to your body’s needs instead of pushing through them.
Emerging research also shows that mindfulness can reduce pain catastrophizing, particularly in conditions like dysmenorrhea and endometriosis.[9]
Why this matters
Stress, emotional wellbeing and nervous system regulation all play a role in how your cycle shows up each month. When you start supporting your body through practices like yoga, breathwork and mindfulness, you’re not just managing stress; you’re actively supporting your hormonal health.
This is what body literacy looks like in practice: understanding your signals, working with your biology and creating conditions where your body can function at its best.
References
Toufexis, D., et al. (2014). ‘Stress and the reproductive axis’. https://pmc.ncbi.nlm.nih.gov/articles/PMC4166402/
Tilbrook, A. J., et al. (2000). ‘Stress and reproduction: central mechanisms and sex differences in non-rodent species’. https://pubmed.ncbi.nlm.nih.gov/12186687/
Gordon, C. M. et al. (2017) Functional Hypothalamic Amenorrhea: Endocrine Society Clinical Practice Guideline https://academic.oup.com/jcem/article/102/5/1413/3077281
Shufelt, C. L., et al. (2017). ‘Hypothalamic Amenorrhea and the Long-term Health Consequences’. https://pubmed.ncbi.nlm.nih.gov/28658709/
Pascoe, M. C., & Bauer, I. E. (2015). ‘A Systematic Review of Randomised Control Trials on the Effects of Yoga on Stress Measures and Mood’ .https://www.researchgate.net/publication/280028050_A_Systematic_Review_of_Randomised_Control_Trials_on_the_Effects_of_Yoga_on_Stress_Measures_and_Mood
Tsai, S.-Y. (2016). ‘Effect of yoga exercise on premenstrual symptoms among female employees in Taiwan’. https://pmc.ncbi.nlm.nih.gov/articles/PMC4962262/
Miri, H., Rezaeipor, H., & Zareiyan, A. (2024). The effect of a course of yoga exercises on menstrual pain and distress in women with primary dysmenorrhea with and without lumbar hyperlordosis. https://brieflands.com/journals/jamm/articles/156368
Russo, M. A., et al. (2017). ‘The physiological effects of slow breathing in the healthy human’. https://publications.ersnet.org/content/breathe/13/4/298
Taren, A. A., et al. (2015) . ‘Mindfulness meditation training alters stress-related amygdala resting state functional connectivity: A randomized controlled trial’. https://www.researchgate.net/publication/277777439_Mindfulness_Meditation_Training_Alters_Stress-Related_Amygdala_Resting_State_Functional_Connectivity_A_Randomized_Controlled_Trial
Clark Donat, L.E. et al. (2022). ‘The effects of a brief mindfulness-based intervention on pain perceptions in patients with chronic pelvic pain: A case series’. https://pmc.ncbi.nlm.nih.gov/articles/PMC8760341/